 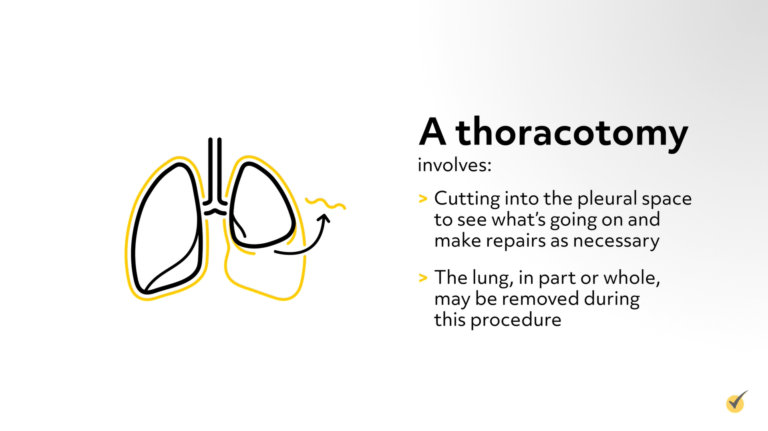
Central venous catheterization increases the risk of pneumothoraces when placed in the internal jugular or subclavian. The rate of iatrogenic pneumothoraces is increasing in US hospitals as intensive care modalities have increasingly become dependent on positive pressure ventilation and central venous catheters. Traumatic and tension pneumothoraces are more common than spontaneous pneumothoraces. Traumatic and tension pneumothoraces are life-threatening and require immediate treatment. Knowledge of necessary emergency thoracic decompression procedures is essential for all healthcare professionals. Įarly recognition of this condition is life-saving both outside the hospital and in modern ITUs. It is most commonly encountered in the prehospital, emergency department, and intensive therapy unit (ITU) settings. It is a severe condition that results when air is trapped in the pleural space under positive pressure, displacing mediastinal structures and compromising cardiopulmonary function. 
Tension pneumothorax is an uncommon condition with a malignant course that might result in death if left untreated. Pneumothoraces are classified as simple (no shift of mediastinal structures), tension (shift in mediastinal structures present), or open (air passing through an open chest wound). 
Atraumatic pneumothoraces are further divided into primary (unknown etiology) and secondary (patient with an underlying pulmonary disease). Iatrogenic pneumothorax is a traumatic pneumothorax that results from injury to the pleura, with air introduced into the pleural cavity secondary to a diagnostic or therapeutic medical intervention. Traumatic pneumothoraces occur secondary to penetrating or blunt trauma, or they are iatrogenic. Pneumothoraces can be traumatic or atraumatic. This places pressure on the lung and can lead to its collapse and a shift of the surrounding structures. The air is outside the lung but inside the thoracic cavity. doi:10.2471/BLT.20.Pneumothorax is the collapse of the lung when air accumulates between the parietal and visceral pleura inside the chest. Smoking and epidemics of respiratory infections. Sitas F, Harris-Roxas B, Bradshaw D, Lopez AD. National Heart, Blood, and Lung Institute. Chronic obstructive pulmonary disease: diagnosis and management. Inspiratory crackles-early and late-revisited: identifying COPD by crackle characteristics. Melbye H, Solis JCA, Jacome C, Pasterkamp H. Respiratory sound classification for crackles, wheezes, and rhonchi in the clinical field using deep learning. Sarkar M, Madabhavi I, Niranjan N, Dogra M. Wheezes, crackles, and rhonchi: simplifying description of lung sounds increases the agreement on their classification: a study of 12 physicians' classification of lung sounds from video recordings.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
